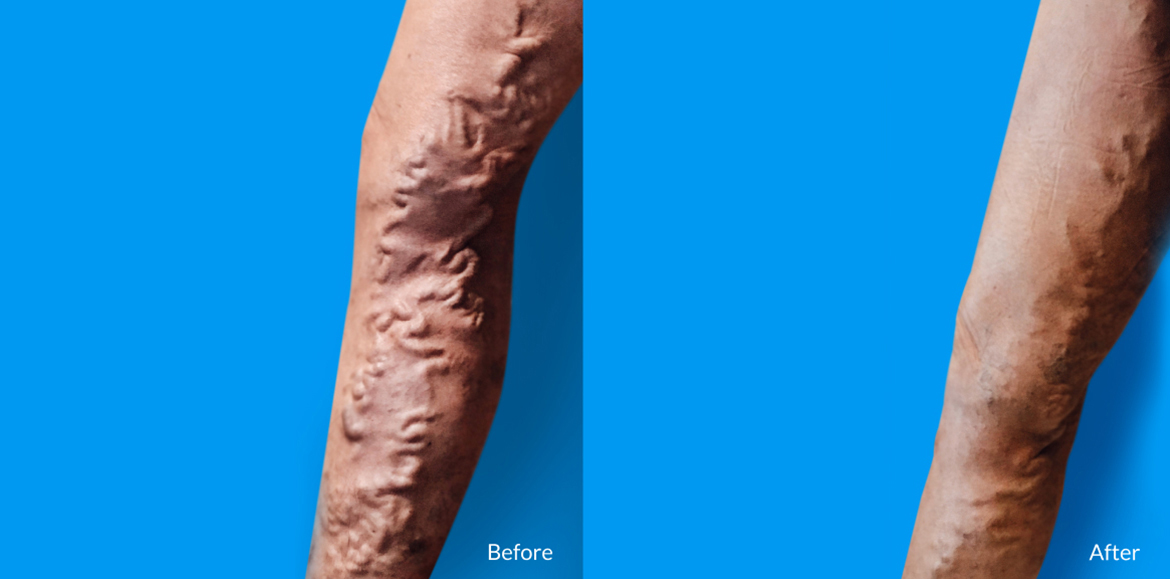
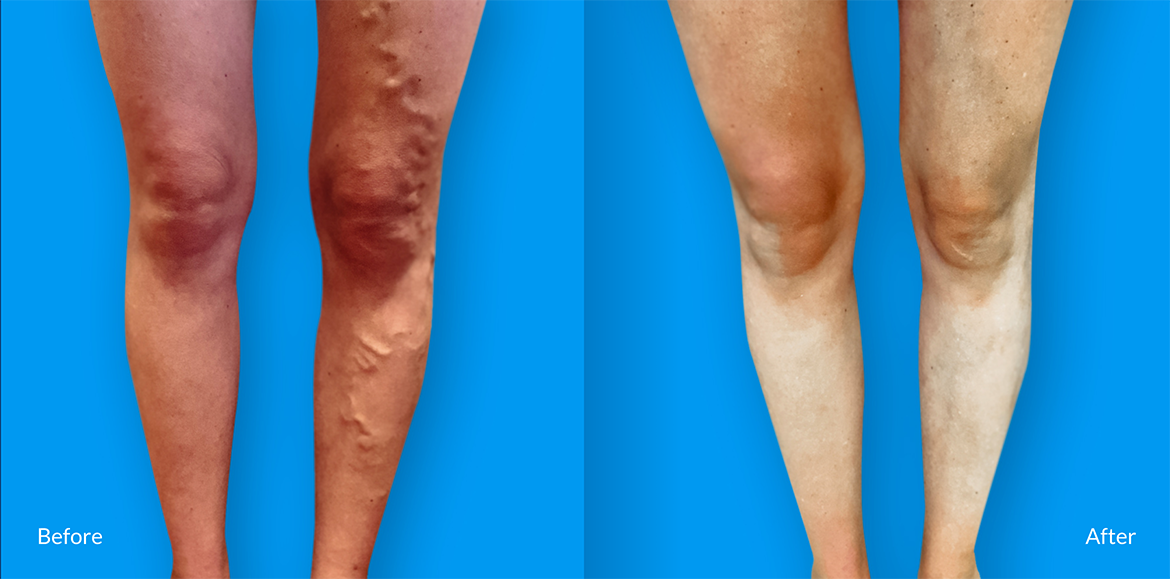
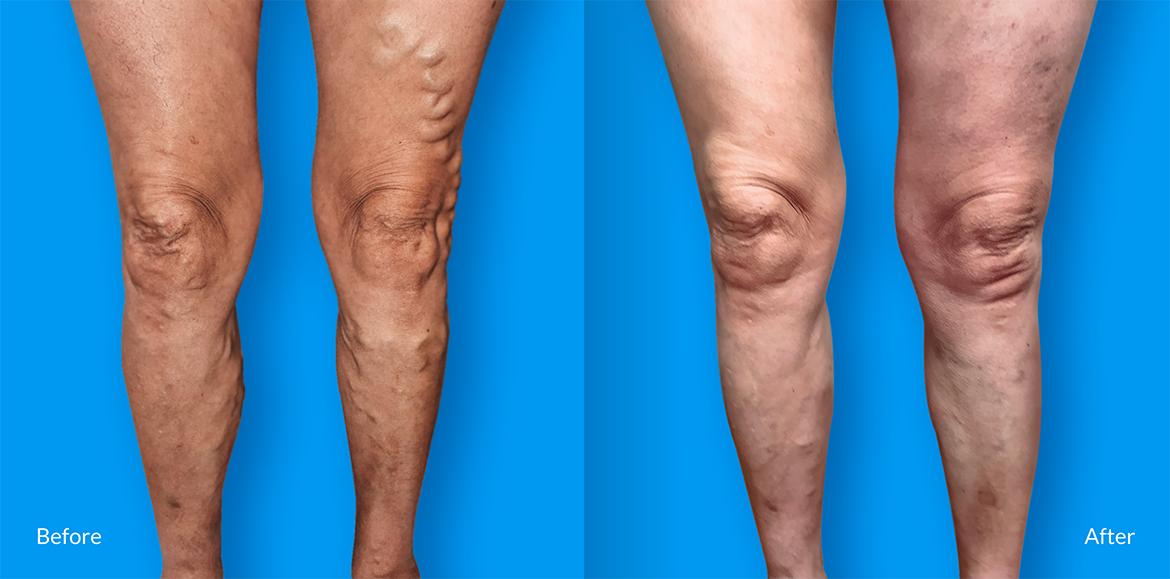
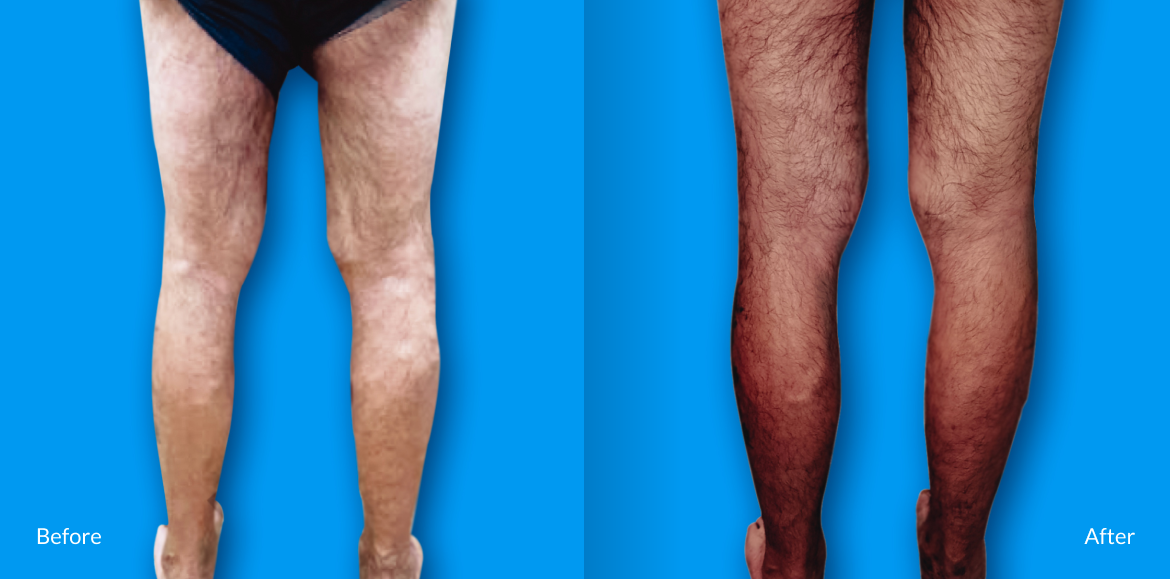
Healthy, beautiful legs lead to an active lifestyle!
Look and feel your best
Vein, Vein, Go Away!TM
A little bit about us
Improving your quality of life is instrumental to our success. We know that you deserve the best, which is why we are always looking for the safest and most effective way of taking care of our patients.


We are the only accredited center in San Diego!
A team of specialists

Mehran Moussavian, FAAC
CEO
Mehran Moussavian, FAAC
CEO
Dr. Moussavian is an extremely talented cardiologist board certified in interventional cardiology, general cardiology and internal medicine. He completed his Internal Medicine residency at the prestigious Yale University including an additional year as chief medical resident and assistant professorship thereafter. He went on to pursue his general and interventional cardiology training at Scripps Green Hospital and Research Foundation where he stood out as a top fellow, selected to become the chief cardiovascular fellow in his final year. He now practices the most cutting edge, minimally invasive surgical procedures with excellent results. In addition to clinical cardiology, Dr. Moussavian’s varied interests include prevention and treatment of peripheral vascular diseases, and stroke prevention. He is also an active participant in multiple clinical research trials and respected speaker and lecturer within the cardiology community.

Lisa Alvarez, PhD, FNP-BC
Nurse Practitioner, Vein Specialist
Lisa Alvarez, PhD, FNP-BC
Nurse Practitioner, Vein Specialist
Lisa Alvarez is a Board Certified Family Nurse Practitioner with a subspecialty in cardiac and vascular disease. Originally from Eastern North Carolina, she completed her undergraduate from UNC-Chapel Hill. She then continued her education completing her Masters and ultimately her Phd from the University of San Diego. She focuses her time co-directing San Diego Vein Specialist where she is certified and coordinates the most up to date and comprehensive care for venous disease. Lisa also spends time with her two children and is an avid hiker and traveler. She is excited to be a part of the SD VEIN team and assures the most advanced care in cardiac and vascular care.

Lyndsay Silver, MSN, FNP-C
Nurse Practitioner, Vein Specialist
Lyndsay Silver, MSN, FNP-C
Nurse Practitioner, Vein Specialist
Lyndsay is a nurse practitioner with nearly 20 years of healthcare experience including hospital, clinic, and specialty care. After graduating from the University of Arkansas with her Bachelors of Nursing she immediately began working at Vanderbilt Children’s Hospital as an RN. She went on to receive her Masters in Nursing from Vanderbilt University while working in Vanderbilt University Medical Center’s Surgical Intensive Care Unit. After graduation she continued to work in critical care and served as an adjunct clinical professor for Kapiolani Community College. As a Nurse Practitioner she has held positions in cardiology at Kaiser Permanente, Honolulu; adult primary care at San Ysidro Health Center; and currently serves in the sub-specialty of vein care at San Diego Vein Specialists. Lyndsay loves to travel and engage people of other cultures. She has served as a short term nurse in Guatemala, Venezuela, Haiti, and Sweden and has done consulting in Pakistan. Lyndsay loves the outdoors and has joined in search and rescue operations in the back country of Colorado in the past. She currently volunteers for the Options for Recovery program, teaching foster parents how to care for high-risk infants. Her most recent and rewarding adventure is that of parenting Ricky, Ella, and Dominic, who continue to challenge and delight. Lyndsay is authentic, engaging, and professional. She is fluent in Spanish and she is passionate about helping her patients have healthy, energetic legs so they can live healthy, energetic lives.

Iran Felix, FNP-C
Nurse Practitioner, Vein Specialist
Iran Felix, FNP-C
Nurse Practitioner, Vein Specialist
Iran Felix is an AANP Board Certified Family Nurse Practitioner. She completed her undergraduate degree from San Diego State University and obtained her master’s degree as a Family Nurse Practitioner at Azusa Pacific University. Iran’s experience as a nurse practitioner has been mainly focused on Peripheral Vascular Disease with an emphasis on chronic venous insufficiency.

Melody Salgado, MSN, AGAC-NP-BC
Nurse Practitioner, Vein Specialist
Melody Salgado, MSN, AGAC-NP-BC
Nurse Practitioner, Vein Specialist
For more than 20 years, Melody’s passion has always been to provide a place of support for her patients by providing a natural solution to help them change how they see themselves and live a happier, more fulfilling life. Melody’s desire is centered around empowering her patients to feel beautiful and to be the best version of themselves. “They are the heart and soul of all I do.”
As a Board-Certified Nurse Practitioner, her philosophy has been to drive continuous energy into providing her patients a high level of care- one that brings clarity and a sense of comfort in knowing their options and what to expect. Education has been a big part of Melody’s life. She received her undergraduate degree from Luzon University and obtained her master’s degree as an Adult Gerontology Acute Care Nurse Practitioner at Walden University.
Raised in San Diego, California, she has three beautiful children whom she is very proud of. As technology is evolving; we find joy in keeping current with cutting-edge advancements and utilizing the most relevant methodologies in our practice. Our patients’ satisfaction and safety are paramount, and we earn their trust by carefully guiding them through the choices and benefits of several state-of-the-art treatments we offer.
SERVICES
Medical/Surgical Treatment
Our medical and surgical treatments are geared toward alleviating the symptoms that you are experiencing due to veinous insuffiency.
SERVICES
Cosmetic Treatment
Cosmetic treatments are expected to reduce the appearance of spider veins and small varicose veins. These treatments may also relieve various symptoms.
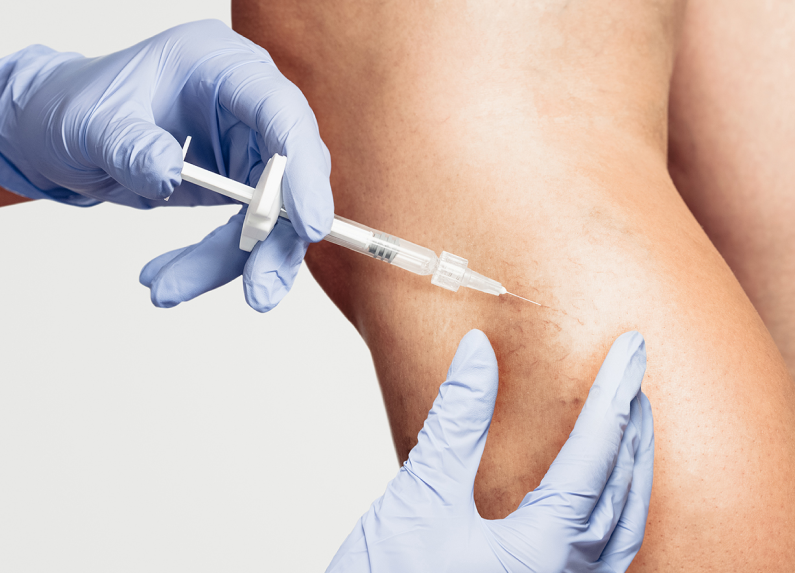
Lifestyle changes
A more conservative way of addressing varicose veins, spider veins, and other veinous insufficiencies. Changing your diet or increasing exercise can significantly lessen the pressure on your legs and improve blood flow in the veins. These lifestyle changes will not get rid of existing varicose veines, but may prevent new ones from forming.
Want to know which treatment
is right for you?
Featured Testimonials
I can’t believe how simple the procedure was and how much better I feel.
The results of the EVLT procedure really exceeded my expectations.
Since the EVLT procedure, I really have not had any pain. My legs looks great and I think I can thank the EVLT system for that.
Las oficina están muy bien distribuida, al access tal cuarto de revisión todo mundo muy amable, la doctora llego a tiempo se hizo el procedimiento y termino en el tiempo requerido, estoy muy satisfecha con los resultados y la rapidez de mi consulta.
100% satisfied with my care at this facility. I highly recommend Dr. Lisa Alvarez and Lyndsay Silver to take care of your veins.
Staff is always so friendly and helpful. Dr. Lisa Alvarez is the best!
Dr. Lisa Alvarez and her team are AMAZING!! Truthfully, I came to this vein specialist just wanting to focus on a cosmetic issue (bulging vein) that I had in my leg. Her team was very thorough and with a bilateral ultrasound of both of my legs, they found a significant… Read More
The Staff is always extremely helpful and kind! All the Specialists are caring and very attentive! Definitely recommended.
Great Staff, they answered my concerns in a very nice way, Dr. Alvarez is amazing
Location is always very clean and great measures taken through this pandemic. Staff is very polite. Dr Lisa Alvarez & Lyndsay Silver are great. She took care of my vein needs and much more. Thank you for always being so polite and attentive to my needs.
7 locations across san diego for your convenience
Escondido
San Marcos
El Cajon
San Diego
Chula Vista West
Chula Vista East
Hillcrest
Don't just trust the beauty and feel of your legs to anyone
San diego vein specialists news
Sign up today to receive the latest information from SD Vein Specialists in your inbox
"*" indicates required fields